
The most common pain complaints encountered are related to the spine. The sources of spinal pain are now well known through the research of the last few decades. The spinal canal is formed by individual bones called vertebra. These vertebra protect the spinal cord and the nerves that exit the spinal cord through openings between the vertebra. These vertebra articulate, or meet, eachother at three distinct joints which allow movement. The disc joints are found just in front of the spinal cord and the paired facet joints are found behind the spinal cord. It is these joints which are subjected to constant wear and tear, stress and strain, with daily living and which are effected by the normal aging changes associated with all joints (degenerative osteoarthritis). These are joints which can become injured or inflamed and which can cause chronic pain. Derangements of these joints can also cause pressure or inflammation of the spinal cord or exiting nerves causing extremity pain as well (often called sciatica in the leg).
The treatments which can alleviate spinal pain are directed at these joints or at the small nerves through which the pain travels from these joints back to the spinal cord on the way to the brain. Utilizing live x-ray, or fluoroscopy, pain management physicians are able to reduce pain from involved spinal joints through injections of minute amounts of steroids directly into or adjacent to the joints felt to be the source of pain. If these are ineffective or do not give prolonged relief, the pain can be reduced through injections of local anesthetic and steroid on the nerves through which the pain is travelling to the spinal cord.
If prolonged pain relief is not achieved in this manner, these injections, or nerve blocks, also serve to predict the ability of the pain physician to obtain long term relief utilizing methods which stop these nerves from functioning through the application of heat in a very safe and controlled manner.
All of these pain relieving treatments have the advantage of having excellent risk/benefit ratios (risk being minimal while the chance of benefit is excellent). Another distinct benefit of these treatments is the ability of the pain management physician to safely repeat the treatment in the future if prolonged relief is obtained.

The field of interventional pain management has evolved substantially over the past decade. This is primarily due to the increased ability of physicians who specialize in interventional pain management to pinpoint the cause of spinal pain through the use of MRI’s and the performance of diagnostic injections and nerve blocks. This has expanded the ability of interventional pain physicians to safely and effectively treat lower back and neck pain with minimally invasive procedures.
Minimally Invasive Procedures
The SPRINT® PNS System is a short-term, 60-day treatment designed to deliver lasting pain relief.
No surgery. No medications. No permanent implants. Just the chance to feel more like yourself again and get back to the life you love.
From low-back and knee pain to persistent headaches, pain can keep you from fully participating in the life you want. It doesn’t have to stay that way.
SPRINT PNS has been used to treat:
- Moderate-to-severe acute and chronic pain
- Non-operable joint pain
- Postoperative pain
- Post-amputation pain
- Neuropathic pain
- Pain due to nerve trauma
How SPRINT PNS works:
During the 60-day treatment period, the SPRINT PNS System sends tiny electrical pulses through the MicroLead placed near the target nerve. This stimulation is believed to interrupt the pain signals, boost healthy non-pain signals, and help rebalance the information the brain receives.
Over time, stimulation of a peripheral nerve with SPRINT PNS is believed to change how your brain may perceive and respond to pain.
Pain relief backed by extensive clinical research – The SPRINT PNS System is supported by more clinical data than any other PNS device available.

The Minuteman® offers a less invasive alternative to traditional fusion procedures. When it comes to stabilizing the spine, the Minuteman® has been shown to be comparable to screws and rods. This helps alleviate symptoms of back and leg pain.
During this procedure, a 1-inch incision is made on the side of your body, dilation is used to access the spine, and the Minuteman® is implanted with bone graft.
The advantages of this approach are that it does not require dissection or retraction of the sensitive back muscles, bones, or nerves. This may lead to a shorter operative time, less blood loss, reduced hospital stay, and a faster recovery time.

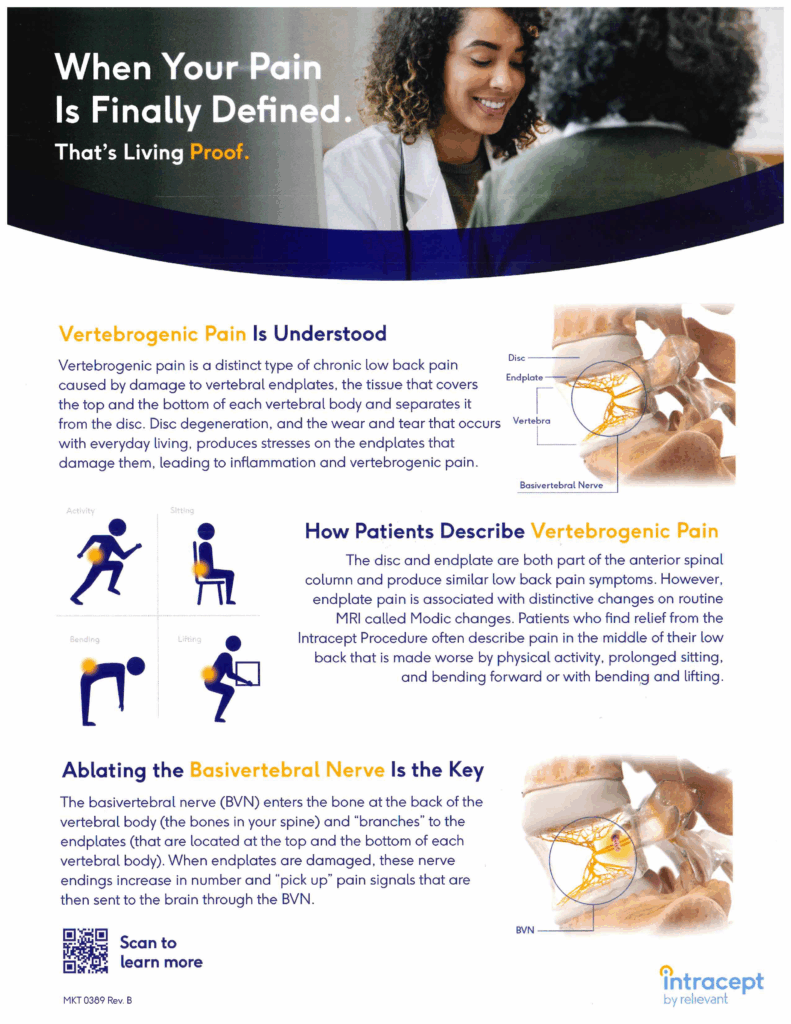
The Intracept Procedure is a minimally invasive procedure that targets the basivertebral nerve for the relief of chronic low back pain.
Intracept Procedure Provides Durable Relief of Vertebrogenic CLBP
Key Benefits of Intracept Procedure:
- Provides a treatment option for patients who have not responded to conservative therapy
- Minimally invasive, outpatient procedure
- Implant-free and preserves all future treatment options
- Provides durable relief of vertebrogenic CLBP
Selective Nerve Blocks are performed near the spine to diagnose the specific spinal nerve that is the root source of chronic back and leg pain. This procedure can also reduce inflammation around the selected nerve root, which may decrease or relieve pain.
During the procedure, the patient is usually given a local anesthetic. The physician then locates, under fluoroscopy, a specific spinal nerve root.
A needle is introduced through the skin into the area adjacent to the nerve root, and medication is injected to bathe the nerve root. The medications typically include an anesthetic and a steroid.
Selective Nerve Blocks are performed on an outpatient basis, and the procedure usually takes 30 to 45 minutes.
Caudal Adhesiolysis is a method of epidural injection that can alleviate pain by breaking up scar tissue and freeing entrapped nerves.
This procedure involves accessing the spinal canal through the sacral hiatus (a triangular bone made up of five fused vertebrae forming the posterior section of the pelvis) using a needle. Once the needle tip is confirmed to be in the caudal space utilizing radio-opaque dye, a catheter is inserted and directed under fluoroscopy.
The dye is also used to identify “filling defects,” which indicate the presence of epidural adhesions.
Medications such as hypertonic saline, local anesthetic, and/or steroid are injected during the procedure to treat pain from epidural adhesions, which have been shown to be a cause of lower back pain.
The insertion of the catheter may also create a mechanical disruption of the adhesions, helping to reduce pain. Caudal Adhesiolysis can also be performed with a small scope in place of the catheter, which may aid in the detection of epidural adhesions.
Intra-articular Facet Injections are fluoroscopically guided injections of a local anesthetic and depot steroid into facet joints suspected to be the source of spinal pain.
In the lower back, this type of pain is most frequently related to degenerative disc disease, which places increased stress on the facet joints. In the neck, it is the most common cause of pain following a whiplash-type injury.
Pain originating from the facet joints may also result from conditions such as synovial tears, cysts, hematomas, subluxations, spinal instability, spondylolisthesis, and vertebral compression fractures.
The purpose of the injection is two-fold. Relief of pain from the local anesthetic provides important diagnostic information, allowing the physician to more accurately identify and treat the source of spinal pain.
The steroid component can provide long-term relief of symptoms in many cases. Further treatment is guided by the patient’s response to both the local anesthetic and the steroid.
Radiofrequency Therapy is a form of pain management that uses the precise application of electrical energy to create pulsed or thermal effects. It can be used to treat a variety of diagnoses and symptoms and is considered a safe procedure with a low rate of complications.
The procedure most commonly involves heating a small amount of nerve tissue to interrupt pain signals. When the nerve is heated to temperatures between 140–185 degrees Fahrenheit, proteins are damaged and the cell membranes combine, disrupting the nerve’s ability to transmit pain.
Radiofrequency energy is delivered through a specialized probe containing electrodes, which distribute energy directly into the targeted tissue.
Although pain relief may begin immediately after the procedure, it can take up to one month for the full effects to be realized. Relief may be long-lasting; however, the treated nerves can regenerate over time, typically within 9–18 months.
Alternatively, the energy can be applied in a pulsed fashion at a lower temperature (104–108 degrees Fahrenheit) to achieve similar relief. The physician will determine which technique is most appropriate based on the patient’s anatomy and the type of pain being treated.
Discography is a diagnostic procedure used to evaluate spinal discs and identify the source of pain.
This procedure involves placing needles into the disc at the spinal level being studied. Under live fluoroscopy, radio-opaque dye is injected, allowing the disc to be visualized. Intradiscal pressure is also monitored during the procedure.
In many cases, a follow-up CT scan is obtained to provide additional diagnostic information.
There are two key components to the diagnosis. The first is the patient’s response to the injected dye, including whether their typical pain is reproduced.
The second component includes the pressure at which pain occurs, the appearance of the disc, the pattern of dye distribution, and findings from the follow-up CT scan.
Evidence of annular fissures or tears, the degree of disc degeneration, and the correlation with pain reproduction can help guide further therapeutic interventions.
Spinal Cord Stimulation (SCS) is a technique that treats pain by stimulating the sensory portions of the spinal cord with low-amplitude electrical impulses.
This technology has been shown to be highly effective for patients diagnosed with neuropathic pain, including conditions such as RSD/CRPS, diabetic neuropathy, arachnoiditis, post-herpetic neuralgia, and radiculopathy. Candidates for this procedure typically have pain that has not responded to other forms of treatment.
An implanted lead (a linearly aligned array of electrodes), powered by a battery or receiver, is placed in the epidural space near the spinal cord. The system works by interrupting pain signal transmission before the signals reach the brain.
There are several types of stimulation available. Some produce a comfortable tingling sensation, while others are sub-perception, meaning no tingling is felt.
The procedure is typically performed in two stages. The first is a trial stage, in which a lead is placed through the skin under local anesthesia into the epidural space. The lead is connected to a trial screening device that the patient takes home.
After receiving instructions on how to operate the device, the patient goes home for several days to determine whether the electrical stimulation provides sufficient pain relief. If the trial is successful, a permanent system can be implanted, with all components placed under the skin.
Patients typically go home the same day for both the trial and the permanent implantation procedures.
Pain Specialists of Greater Chicago (PSGC) currently provides regenerative therapies in the form of platelet-rich plasma (PRP) for a variety of musculoskeletal conditions, most commonly affecting the knee, hip, and shoulder.
We are also excited to announce that we are actively working to participate in a study utilizing umbilical-derived tissue allografts to provide structural support for joints.
We will notify our patients as soon as this treatment option becomes available.
The MILD® (Minimally Invasive Lumbar Decompression) Procedure is a short, outpatient treatment designed to relieve pain and improve mobility caused by lumbar spinal stenosis.
No major surgery. No implants. No general anesthesia. Just the chance to stand longer, walk farther, and get back to the life you love.
From back and leg pain to difficulty standing or walking for extended periods, lumbar spinal stenosis can make everyday activities challenging. It doesn’t have to stay that way.
The MILD procedure has been used to treat:
- Lumbar spinal stenosis (LSS)
- Neurogenic claudication (pain or heaviness in the legs with walking or standing)
- Thickened ligament causing nerve compression
- Chronic low back and leg pain that has not improved with conservative care
How the MILD procedure works:
During the procedure, a physician uses specialized tools through a very small incision to remove excess ligament tissue that is pressing on the spinal nerves. This helps create more space in the spinal canal and reduces nerve compression, allowing for improved mobility and function over time.
Relief backed by clinical research – The MILD procedure is supported by clinical studies demonstrating meaningful improvements in pain, walking ability, and overall quality of life for patients with lumbar spinal stenosis.

I have been under Dr. Glaser's care for well over 10 years and have had procedures + therapy to keep my back pain in check for most of the time. I typically would have an RF ablation done every 18-24 months combined with other injections. I had an ablation done this past June and it brought some relief but over the last year I had developed continual pain in my lower back that was not getting resolved. Dr Glaser introduced me to "Intracept" and, an MRI showed that I was a candidate for this procedure. I had the procedure done (outpatient) and I was completely functional later in the day. The recovery process was as expected, minimal discomfort (some incision pain) and over the next 2-3 weeks, little by little my lower back pain was completely eliminated. There is a wealth of information on Intracept and the great team at Boston Scientific provided great support throughout. Dr. Glaser has been able to keep me away from surgery and while I don't generally believe in silver bullets, this certainly feels like one. I can't say enough about Dr. Glaser and his team of professionals + the research he continually does on innovative new ways to help his patients. I highly recommend this to anyone who suffers from chronic lower back pain.
Dr. Glaser literally saved my husband’s life. Keith has had back pain for 55 years and countless surgeries on each level of his spine. Doctors have said his spine looked like a fun house. After seeing Dr. Glaser for years of pain, Dr. Glaser introduced my husband to the Intracept procedure. Keith had the Intracept procedure performed in August of 2025 and as of November, 2025, he is in no pain whatsoever. Dr. Glaser is Keith’s and my hero.
